Two-Rescuer CPR: When to Switch and What Changes
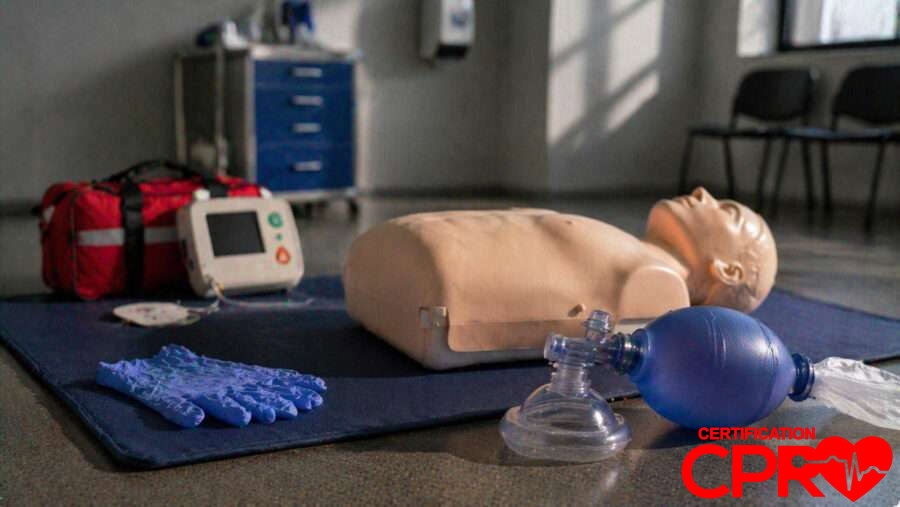
The difference shows up after the first couple of minutes. One rescuer is on the chest, counting and pushing, while the AED is still being opened and someone is trying to remember the next step. The compressions start strong, then the shoulders slow down, the depth gets shallow, and the pause before the next set gets longer than anyone meant it to be.
Two-rescuer CPR exists to prevent that slide. Once a second trained person is available, the response stops living in one body. One person handles compressions while the other helps with breaths, the AED, timing, and the switch itself. That split matters because compression quality usually starts dropping before the rescuer notices it.
This comes up in any setting where two trained people may be present at the same time: a dental practice, a school with multiple BLS-certified staff, or a business that runs regular onsite CPR training. It also matters in AHA BLS CPR class because high-quality CPR means more than knowing the rate; it means keeping the whole response organized under pressure.
What Two-Rescuer CPR Means
Two-rescuer CPR means two trained people are working the same cardiac-arrest response together instead of one rescuer trying to do everything alone. That changes the response in useful ways because one person can stay focused on strong compressions while the other helps with timing, breaths when appropriate, AED setup, and scene organization.
Upcoming CPR Class Dates and Times
The basic problem does not change: the person is still unresponsive and not breathing normally. You still need 911, CPR, and an AED as fast as possible. What changes is how the work is divided.
One rescuer trying to count, reposition, grab equipment, watch the airway, and keep compressions strong all at once is exactly how compression quality starts to collapse.
What Changes When a Second Rescuer Is Available
The biggest change is that the response becomes more organized. Instead of one person trying to juggle every task, the work gets assigned in a way that protects the most important job: keeping compressions strong and interruptions short.
With two trained rescuers:
- one person can stay on compressions
- one person can manage breaths when the full CPR sequence calls for them
- one person can get the AED ready while compressions continue
- switching can happen before fatigue causes long pauses or shallow compressions
The second rescuer also helps catch things the first rescuer may miss, like pace drifting, leaning on the chest, or compressions getting weaker as the minutes pass.
Two-rescuer CPR consistently produces better compressions. It gives the team a better chance of protecting rate, depth, recoil, and continuity.
Who Does What During Two-Rescuer CPR
Most of the time, one rescuer starts on chest compressions while the other handles the support role. The exact split can vary a little by training context, but the idea is always the same: the compressor compresses, and the second rescuer supports the rest of the response.
That support role may include:
- opening the airway when breaths are part of the response
- giving rescue breaths if appropriate
- attaching AED pads
- clearing the patient during analysis and shock
- counting out loud
- watching for fatigue and helping cue the switch
The exact split can depend on the training context and the age group involved, but the bigger point stays the same: each rescuer has a defined job, and that keeps the response smoother.
When people are both half-doing everything, pauses get longer and the scene gets messy fast.
When to Switch Rescuers
Rescuers should switch about every 2 minutes, or about every 5 cycles of 30 compressions and 2 breaths, and sooner if the compressor is clearly getting tired. You do not wait until compressions are already weak and sloppy before admitting it is time to rotate.
The reason for the switch is simple. CPR is tiring. Even a rescuer who feels fine at the start can lose depth, pace, and recoil faster than they realize, especially once a couple of minutes have passed.
Switching protects compression quality. It is not a sign anyone failed. The goal is to change positions with as little interruption as possible so the next set of compressions starts right away.
If one rescuer starts fading before the 2-minute mark, switch sooner. The whole point is to protect compression quality, not to force an exact clock if the CPR is already slipping.
How to Switch Without Creating Long Pauses
A good switch is quick and organized. The next compressor should be ready before the change happens, not walking into place after compressions have already stopped. That preparation keeps the pause from stretching longer than it needs to.
That means:
- the off-chest rescuer gets into position early
- both rescuers know when the switch is coming
- the change happens quickly at the planned moment
- compressions resume right away
Long, awkward switches defeat the point. The whole reason two-rescuer CPR helps is that it protects compression quality while keeping interruptions short.
This is also where practice matters. People understand the idea when they read it, but the timing only gets smooth after they have actually done the handoff.
How Breaths Fit Into the Two-Rescuer Response
Two-rescuer CPR can make breaths easier to manage because one person can stay focused on the airway while the other stays focused on compressions. That matters more in the full BLS sequence than it does in simplified public-response messaging, where the instructions are intentionally stripped down for bystanders.
It is also why two-rescuer CPR shows up so clearly in hands-on BLS training. Students learn how compressions, breaths, rhythm, and switching work together instead of trying to bolt the pieces together on their own later.
For lay rescuers in an adult sudden-collapse emergency, the public message still often centers on pushing hard and fast and using an AED. For trained rescuers, the fuller sequence matters, and the second rescuer helps that sequence stay organized.
Why Fatigue and Interruptions Matter So Much
Two-rescuer CPR matters for compression quality, not convenience.
As rescuers get tired, they tend to:
- push shallower
- lose pace
- lean on the chest
- take longer pauses
- fumble transitions
The second rescuer helps prevent exactly that kind of drop. One person buys the other person relief before the quality falls too far, and the whole response stays tighter because fewer steps are being juggled by one body.
This is also why the AED piece matters so much. One rescuer can keep compressions going while the other gets the device ready. If an organization wants multiple responders working from the same pattern, onsite CPR training is usually the better next step.
Where This Fits in BLS Training
Two-rescuer CPR is one of the places where AHA BLS stands out from lighter CPR content. The class teaches more than what CPR stands for or which rate range to remember; it gives people practice with a team response when two trained rescuers are in the room and the patient needs more than a single bystander trying to improvise.
Upcoming CPR Class Dates and Times
AHA BLS is where two-rescuer CPR becomes a practiced skill instead of an idea. Whether the student comes from a clinical setting or simply wants more than the simplified public version, this is where the response is learned with manikins, repetition, and a team to practice with.
Educational note: use this information for general awareness only. It is not a substitute for calling 911, hands-on training, or professional medical judgment during an emergency.
